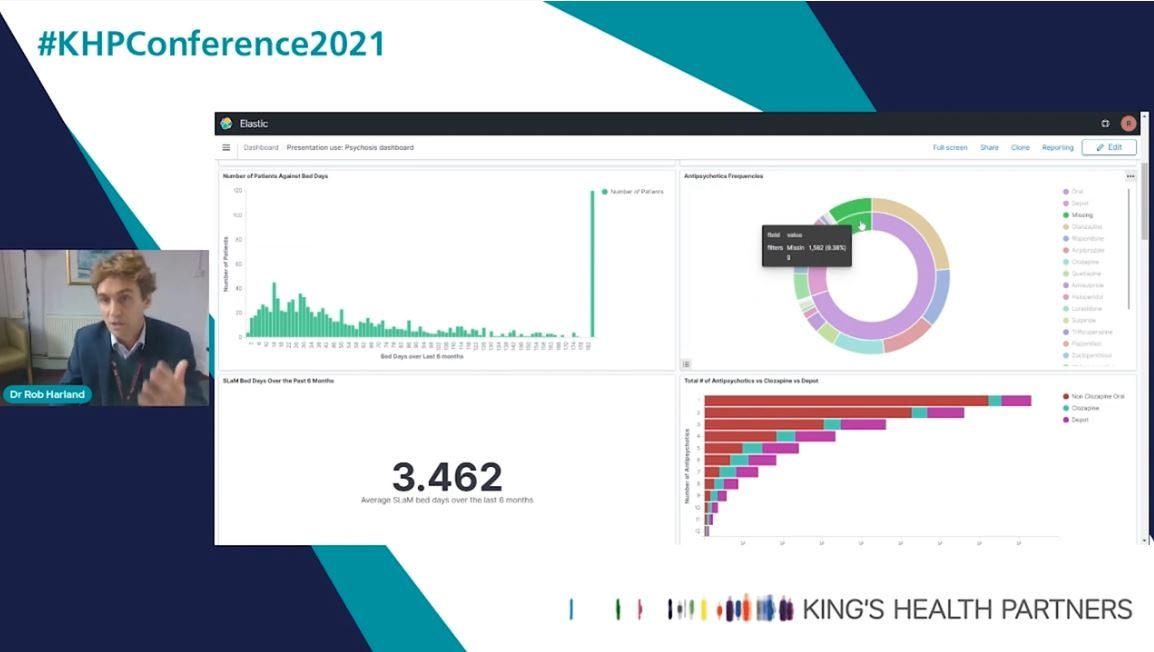
The Psychosis Population Health Management Platform, which was built on CogStack, was presented at the King’s Health Partners annual conference by Dr Rob Harland....
The CogStack team is proud to receive the Public Sector Award of Elastic Excellence 2021 which recognizes a Public Sector organization that is leading the way in innovative, sustainable, and critical...
Black, Asian and Minority Ethnic groups (BAME) hospitalised with the virus have an average age of 63 years and have a high likelihood of hypertension and diabetes. In contrast, the average age of whit...
Zeljko Kraljevic, our research fellow in Health Informatics, wrote three articles on Medium about MedCAT tutorial on analysing Electronic Health Records (EHR). MedCAT is one of the CogStack's...
Yesterday, three of our Radar-base team members (Pauline Conde, Yatharth Ranjan, and Zulqarnain Rashid) participated at the South London and Maudsley (SLaM) Staff Conference 2020....
Secretary of State for Health and Social Care, Matt Hancock MP, highlighted CogStack during his keynote address to the Health Tech Alliance, 28 January 2019....
NHSX recently released a report into the state of AI in healthcare, where they see practical applications for this tech, and what they're doing to build ethics, transparency and NHS values into the wa...
Around 300 delegates including researchers, clinicians, service users and members of the local community gathered yesterday for the NIHR Maudsley BRC's Annual Conference 2019....
New collaborative research programme will explore potential of wearable devices to help prevent and treat depression, multiple sclerosis and epilepsy. A major new research programme supported by th...
Science Business article on big data in health quotes Dr Richard Dobson. Fears big data could affect insurance coverage and be used to track the performance of clinicians are holding back adoption....